Burnout at work could be caused by a lack of role clarity regarding responsibilities and scope, unfair treatment at work, poor or lack of communication and/or support from managers, unreasonable time pressure, and last but not less important, an unmanageable workload. Burnout among healthcare personnel occurs during the pandemic due to an overwhelming workload. The cause(s) of each person’s burnout must be considered while developing solutions and strategies to prevent burnout in healthcare professionals. The key to preventing and treating burnout in the healthcare industry is identifying the cause or causes and working to develop emotional intelligence. This article addresses the issue of workplace burnout and suggests solutions to ways to prevent burnout at work. Having high emotional intelligence is associated with better mental health, better social problem-solving, superior relationship quality, and higher academic and professional achievement, according to scientific research. To improve mental health and minimize burnout, we include several tips to prevent burnout.
Table of Contents
Causes of Burnout at Work
Burnout at work could be caused by:
- lack of role clarity regarding responsibilities and scope,
- unfair treatment at work,
- poor or lack of communication and/or support from managers, and
- unreasonable time pressure
- unmanageable workload
Burnout in Healthcare
During the pandemic, the unmanageable workload causes burnout in healthcare professionals. To think about the strategies to prevent burnout in healthcare, it is needed to about the cause/s of the burnout of each individual. Eliminating the cause/causes and working on improving emotional intelligence is the key to preventing burnout in healthcare professionals and curing them.
In this article, we discuss this problem and the ways to prevent burnout at work. According to scientific evidence, having a high emotional intelligence (EI) is linked to greater mental health, improved social problem-solving, superior relationship quality, and higher academic and occupational success.
As a result, educators and consultants have invested a lot of time and energy into creating tools that will encourage EI. Therefore, we include several tips to prevent burnout by improving mental health and lifestyle change.

Let’s start.
The SARS-CoV-2 (COVID-19) pandemic has been a tsunami of planetary magnitude, unexpected, unknown, unpredictable, and deadly. It has created an extraordinary healthcare situation in all countries of the world.
The enormous work overload to which healthcare professionals have been exposed, the significant emotional burden, stressful situations, and the fear of contagion for themselves and their families, among other aspects, have had an impact on professionals, turning them into second victims.
We are beginning to have an idea of its magnitude, not only in terms of health, but also bio-psycho-socially, but we still have a lot to know, and there is much that we may never know. Even at the quantitative level: deaths due to COVID in impoverished countries of the world, undiagnosed deaths in all types of countries, secondary mortality and morbidity due to overloading of health systems, in oppressed groups: children, women victims of violence, psychologically, biologically or socially fragile patients, the precariat, the impoverished masses of the countries of the South.
Many of these effects are showing up more than a year and a half later, particularly, those related to mental health impairment. The pandemic has changed the lives of all of us: especially those who have lost their health or the lives of family members. And all of us, but primarily children and adolescents, have seen our daily activities, emotions, and relationships change. But in this pandemic, those who are most affected are those who are most needed to ensure the care of people and the sick: healthcare workers, especially healthcare workers.
In fact, the pandemic is having an unequal impact according to sex and gender, as recognized by national and international experts, who urge the collection of sex-disaggregated data and its analysis with a gender focus.
At this point it is unquestionable to recognize:
- That the COVID-19 pandemic represented a global social, economic, and health turning point.
- This highlighted the shortcomings of a health system that had already been severely punished.
- That this prolonged situation of work-related stress significantly affected the physical, mental, and emotional health of everyone in general and of healthcare professionals in particular.
- The inherent characteristics of work in the health field indeed determine a context prone to instances of high stress given the nature of the activity and the frequent imbalance between external demands, self-demand, and often the resources available to meet the objectives efficiently.
- When the mechanisms for managing these situations are inadequate or insufficient, maladaptive responses arise as a consequence, represented by emotional exhaustion, the feeling of a low sense of achievement, and depersonalization towards patients, which define in the worker the perception of being “burned out by work”, also known as burnout syndrome.
- The intensity and uncertainty of the events of the last 2 years determined in health professionals that the prolonged and continuous confrontation of these situations became in itself a burden that generated in some cases, and increased in many others, symptoms of emotional exhaustion, frustration, and lack of motivation for the profession, symptoms of emotional exhaustion, frustration and lack of motivation for the profession.
Primary care, despite being one of the fundamental pillars of the healthcare system, has also been and continues to be severely affected. It is well known that, in addition to the usual shortage of time for consultations, there is the incessant flow of protocols, the increase in administrative tasks, social distancing, the fear of contagion, the fear of error, and, very importantly, the constant feeling of not practicing the profession as one would like to and the lack of attention to other patients.
Let’s see the Strategies to Prevent Burnout in Healthcare
Strategies To Prevent Burnout In Healthcare
When a professional or another worker feels that he/she does not receive sufficient institutional and peer support, when he/she has very limited control over his/her work, when resources are not available, or when he/she is faced with demands and needs, making decisions based on criteria beyond his/her control, this provides fertile ground for professional burnout, with the negative impact that this has on the workers’ health and patient care.
However, tackling the crisis and its root causes alone is not enough, and significant steps to address the crisis and its root causes must be taken at a systemic and institutional level with concrete efforts by all stakeholders.
Strategies to Prevent Burnout in Healthcare: The proposals must be realistic and adaptable, and not limited only to attractive statements that are not implemented.
Strategies to Prevent Burnout in Healthcare: Establishing team meetings, creating opportunities to review and learn from what has been experienced, creating care plans, individual or collective leadership strategies, and requesting external support (a psychologist, a coach, or another) are very important. But they lose value and usefulness if they are not supported by adequate staffing and resources in the health centers, if the needs of the professionals are not listened to and acted upon, and if the new specialists in training are not motivated so that they will also be the ones who in the future exercise their profession with satisfaction and without burning out.
Strategies to Prevent Burnout in Healthcare: From a neuroscientific and relational perspective of emotions in groups, the prominent emotions with COVID were initially fear and feelings related to the rupture of attachment (e.g., solidarity). Later, to the extent that sadness has been largely stolen from the population and solidarity has been marginalized, the predominant emotions have been anger and separation anxieties, with large doses of incontinence and mass psychosocial repercussions, even in supposedly “educated” countries. Often, these emotional reactions, inadequately potentiated or contained, have been transformed into violence in some and into hopelessness and apathy in others.
How Can Burnout Be Prevented in Healthcare
In all countries, healthcare professionals have suffered the impact of this unexpected pandemic, and also at the triple biological, social, and psychological levels. We already have data on the impact of the pandemic on the mental health of populations, and studies and reflections on the impact on healthcare workers are beginning to appear, with the usual announcements of an increase in anxiety, depression, and stress disorders.
Strategies to Prevent Burnout in Healthcare: One of the first Spanish studies, carried out after 4,145 surveys, points to a notable worsening of the state of self-perceived health, of the quantity and quality of sleep, 30% of sick leave in nurses, and 20% of physicians, 57% of physicians reporting physical exhaustion and 48% emotional exhaustion (19 and 18.6% before the pandemic, respectively), as well as an increase in the ideation of leaving the profession and early retirement.
As we pointed out months ago, in these situations of social and political crisis it is easy to attribute all emotional suffering to “mental disorders” or, even worse, to “mental illness”, contributing to the medicalization and psychiatrization of the population. This is also true of health professionals, especially those in emergency, intensive care, and primary care services, and a veritable wave of “mental disorders” is predicted for them, although sometimes ad hoc terms such as “professional burnout”, burnout and the like are used: of course, poorly elaborated emotional and psychosocial pressures are the basis of burnout, even though they may (or may not) be based on underlying mental disorders. But, from the theory of grief and trauma processes, the effects of a stressor or trauma vary not only with the power, duration, and characteristics of the stressor, but also according to the psychosocial context in which it affects, and according to the sex and psychological characteristics of the subject or group subjected to the trauma or stress. At the primary care level, morbimortality has been especially important. Illnesses, sick leave, shift changes, and work overload have had a direct impact on the emotional state and mental health of professionals (especially health professionals), their families, and their practices.
Strategies to Prevent Burnout in Healthcare: If we want to reflect and rethink the future on an updated basis, we cannot fail to take into account the psychological components, personal and group, that make a conflict, loss, or stress lead (or not) to a “mental health decompensation”, a mental disorder or burnout. From now on, we must rethink and reflect on the personal equipment with which we were facing the gradual impoverishment of our public services: with what emotions, with what values, with what attitudes. For example, there is already data showing that teamwork, support, and recognition by the team and managers, as well as occasional collaborations with mental health teams, where they have worked, have helped significantly to maintain and improve the activity of hospital and primary health care (PHC) teams, even amid the pandemic.
We must also investigate to what extent the training received in recent decades by many physicians in “developed” countries favors technocratic, hospital-centric, and privatizing practices instead of community, public health, and preventive practices.
Undoubtedly, today public authorities and professionals must strive to revalue a well-equipped, competent, and prestigious PHC planned and managed to a large extent by the professionals themselves and committed to patients in a renewed relationship framework based on patient autonomy, co-responsibility, and trust.
The Role of Emotional Intelligence in Curing and Preventing Burnout at Work
Emotional intelligence is understood as the ability to know one’s own and others’ emotions. While we all need to work and grow our emotional intelligence, let’s imagine roles within a hospital and staff dedicated to the health of patients.
Even without a pandemic, the emotional intelligence of critical care nurses is a necessary competency in job performance.
The relevance of emotional intelligence in the professional experience, in emotional exhaustion and burnout prevention, in increasing patient safety culture, in contributing to organizational citizenship behavior, and in resilience.
Emotional intelligence is an essential competency of healthcare personnel, especially those engaged in critical care, at all times (even without the COVID-19 pandemic) with repercussions at the professional, personal, and organizational levels.
The healthcare crisis has turned healthcare professionals into the second victims of SARS-CoV-2. Their detection is essential to offer them the necessary resources and help to guarantee their emotional well-being, eliminating barriers and helping them to emerge stronger.
Burnout is a growing problem with significant financial and emotional repercussions. If treatments are started earlier on, I think burnout can be avoided. It will be necessary to focus more on preventative techniques than coping mechanisms for such upstream interventions to be successful.
Remarkably, the majority of burned-out workers continue to work. This implies that we are accountable for ensuring its safety regardless of whether it’s a real or virtual location they access every day. Instead of just providing greater protection, we need to take proactive steps to create an environment that is healthy and devoid of the toxic elements that are causing their exhaustion.
This will need effort, including organizational analysis as well as more study and testing of novel ideas and strategies that have the potential to improve both well-being and financial results. It will need us to reevaluate the way we now approach burnout and develop a strategy that strengthens our responsibility and does away with the demand that employees fight fatigue on their own.
Although “emotional intelligence” (EI) is one of the most often used psychological words in common nomenclature, there is heated discussion about its construct, variance, and predictive validity.
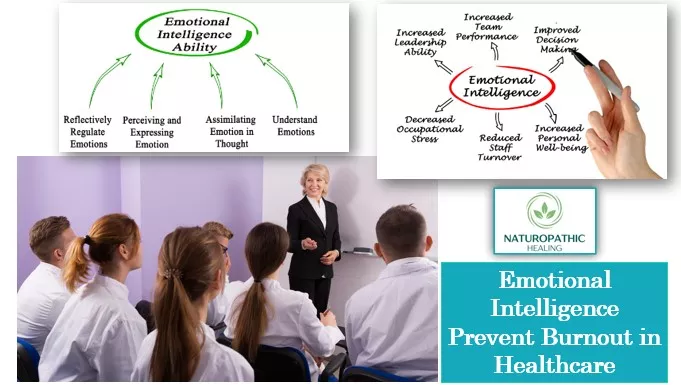
Despite this controversy, the emotional intelligence construct is made up of a set of skills that unquestionably affect significant social and personal outcomes. These skills include recognizing emotional states in oneself and others, using emotions to guide thought and behavior, understanding how emotions shape behavior, and emotion regulation.
Many scientific neuropsychological findings might support efforts to define and quantify EI.
Healthcare practitioners need to possess emotional intelligence as a skill and a personality attribute. The wellness of persons who practice mindfulness meditation has been shown to increase, resulting in higher mental health, self-care, and work satisfaction. Several academic investigations showed a link between emotional intelligence, specifically the ability to control emotions, and mindfulness. Moreover, emotional tiredness has a negative correlation with mindfulness.
The promotion of emotional equilibrium, emotional awareness, emotional acceptance, emotional recognition, expressive repression, and a decrease in emotional tiredness have all been demonstrated as benefits of training programs based on mindfulness.
Research shows that strong emotional intelligence is connected with greater mental health, better social problem-solving, superior relationship quality, and higher academic and professional success. As a result, educators and consultants have worked hard to create methods that enhance EI.
As emotional regulation impairments have been associated with aggressive behavior, anxiety, and depression, emotion management is a skill that is essential to mental health and social functioning.
Tips To Prevent Burnout at Work
In addition to mental burnout, physical stress reduction is key. That is why it may be advisable to review the diet since it is common that in situations of stress and fatigue, we are not receiving adequate food or even a diet that helps us to cope with the processes of physical and mental exhaustion. The posts in the category Foods can be of great help.
How Many Years To Recover From Burnout
On the other hand, the duration of burnout depends on each person. Some people seek to overcome it quickly and look to the future with great confidence knowing that they will prevent it. There are individuals that even though they are no longer in the burnout situation in their mind keep repeating past experiences and seem not to progress. This is where emotional intelligence and the different tools we can have at our fingertips play a key role.
All therapies that help us to connect with ourselves can be useful to overcome this moment.
Reconnecting with the inner self is key to overcoming mental fatigue and energy in a short time, as well as avoiding the depression that can occur after burnout.
This reconnection with ourselves can be achieved in different ways. Some people prefer yoga, forest bathing, sound therapy, meditation, and positive affirmations and others prefer to go for a run. The reality is that there is no formula, but it is necessary to raise the body’s endorphin level, and all of these activities achieve this.
Final Thoughts on the Strategies to Prevent Burnout in Healthcare
Final Thoughts on the Strategies to Prevent Burnout in Healthcare. Lack of job clarity about responsibilities and scope, unjust treatment at work, inadequate or absent management support, unacceptable time pressure, and lastly, but no less importantly, an overwhelming workload, are all potential reasons for burnout at work.
In addition to mental exhaustion, reducing physical stress is essential. As it is typical to under-eat or even have a diet that hinders us from coping with the processes of physical and mental tiredness when we are stressed or tired, it may be wise to check your diet.

The length of burnout, on the other hand, varies from person to person. Others are eager to avoid it and have complete faith in their ability to do so in the future. There are some people who, even though they are no longer burnt out, seem to be stuck in the same old patterns of behavior. Here, emotional intelligence and the many tools we have at our disposal are crucial.
To get over this point, any therapy that encourages us to connect with ourselves might be helpful.
Reestablishing a connection with one’s inner self is essential for overcoming temporary energy and mental exhaustion as well as for preventing the despair that might follow burnout.
There are several strategies to re-establish this reconnection with the inner self. Some individuals choose running, while others favor yoga, forest bathing, sound therapy, meditation, and listening to positive affirmations daily for a couple of months. Even though there is no magic recipe, all of these activities work to increase the body’s endorphin levels.
Emotional intelligence and increasing it is the key to cultivating a healthy style to prevent future burnout. Healthcare professionals must be emotionally intelligent both as a personality trait and a competence. It has been demonstrated that practicing mindfulness meditation improves one’s wellness, leading to improved mental health, self-care, and job satisfaction.
Overall, these are the strategies to prevent burnout in healthcare units.
References to Understand The Strategies to Prevent Burnout in Healthcare
Barbey AK, et al. Lesion mapping of social problem-solving. Brain. 2014;137:2823–2833. [PMC free article]
Brackett MA, et al. Relating emotional abilities to social functioning: a comparison of self-report and performance measures of emotional intelligence. J Pers Soc Psychol. 2006;91:780–795. [PubMed]
Dyrbye L, et al. Effect of a professional coaching intervention on the well-being and distress of physicians: A pilot randomized clinical trial. JAMA Intern Med., 179 (2019), pp. 1406-1414
Feist GJ, et al. Predicting creativity from early to late adulthood: intellect, potential, and personality. J Res Pers. 2003;37:62–88. [Google Scholar]
Fessell D, et al. Coronavirus disease 2019 (COVID-19) and beyond: Micropractices for burnout prevention and emotional wellness. J Am Coll Radiol., 17 (2020), pp. 746-748
Hunter JE, et al. Validity and utility of alternative predictors of job performance. Psychol Bull. 1984;96:72–98. [Google Scholar]
Kee KS, et al. Emotional intelligence in schizophrenia. Schizophr Res. 2009;107:61–68. [PubMed]
Libbrecht N, et al. Emotional intelligence predicts success in medical school. Emotion. 2014;14:64–73. [PubMed]
Moss J. Rethinking Burnout: When Self Care Is Not the Cure. American Journal of Health Promotion. 2020;34(5):565-568. PubMed
Preti E, et al. The psychological impact of epidemic and pandemic outbreaks on healthcare workers: Rapid review of the evidence. Curr Psychiatry Rep, 22 (2020), pp. 1-22
Reyes MR, et al. The interaction effects of program training, dosage, and implementation quality on targeted student outcomes for the RULER approach to social and emotional learning. School Psych Rev. 2012;41:82–99.
Rivers SE, et al. Measuring emotional intelligence in early adolescence with the MSCEIT-YV: psychometric properties and relationship with academic performance and psychosocial functioning. J Psychoeduc Assess. 2012;30:344–366.
Snarey JR, et al. How lower- and working-class youth become middle-class adults: the association between ego defense mechanisms and upward social mobility. Child Dev. 1985;56:899–910.
Xiong J, et al. Impact of COVID-19 pandemic on mental health in the general population: A systematic review. J Affect Disord, 277 (2020), pp. 55-64
